Looking for more news from AbbVie? Follow us on social media.
News
| Su | Mo | Tu | We | Th | Fr | Sa |
|---|---|---|---|---|---|---|
| Su | Mo | Tu | We | Th | Fr | Sa |
|---|---|---|---|---|---|---|
-
April 04, 2024
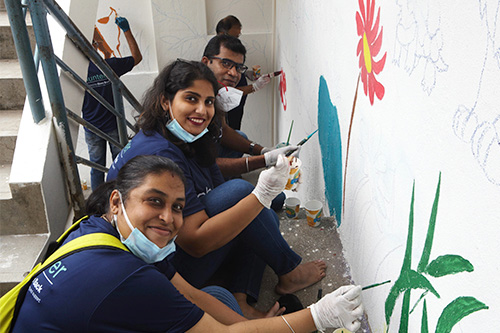 |
Explore where we've been and how we continue to go beyond medicine to make a remarkable impact. Learn more
 |
Our commitment to science is a commitment to better our society. Read our 2022 ESG report
 |
We've been honored to receive some of the most prestigious ratings and recognnitions in the industry. Learn more
 |
See our latest 2023 Annual Report on Form 10-K. Learn more
